No products in the cart.
For everyday aches and athletic demands
Support That Fits How Your Body Actually Feels
Pain shows up differently for everyone. We help you choose support that matches where it hurts, how it behaves and what makes it worse—so you can find what actually fits your needs.
Cushioning, compression, bracing and stability support to help movement feel easier, more comfortable and more confidently supported.

Fast Delivery
Most orders arrive within 1–3 working days.
30-Day Refunds
Extra peace of mind if something is not right for you.
Secure Payment
Protected checkout with all major cards accepted.
Helpful Support
Guidance from a team that understands the range.
Find support by body area
How Your Pain Shows Up Can Help You Choose the Right Support
The way pain behaves often tells you something useful. Discomfort that is sharp on first steps, builds gradually through activity or appears after rest does not always point to the same kind of strain. A knee that feels stiff after sitting is not always asking for the same support as one that feels less steady on stairs or uneven ground.
NuovaHealth is designed to make that process easier to navigate. You can start with the body area that needs support, then narrow down by how symptoms actually behave—because where pain shows up is only part of the picture. The way it feels, when it starts, and what makes it worse often matter just as much.
Use the guide below to explore by body area and find support that fits the way your symptoms actually behave, not just where they happen to be felt.
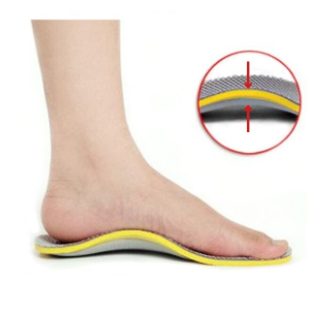
Feet & Heels
Insoles, heel cups, bunion relief and massage tools for first-step heel pain, pressure under the foot, arch strain, running discomfort and tired feet after longer days or walks. This part of the range is focused on easing pressure, improving comfort and making walking feel better supported.
Browse the full footcare rangeAnkles
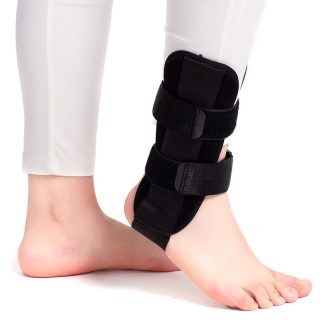
Ankle braces and supports for sprains, weakness, tendon irritation and joints that no longer feel fully reliable. These options are designed to improve stability, protect vulnerable movement and help you feel more secure when walking, training or getting back to activity.
Explore ankle supportsKnees
Knee sleeves, braces and structured supports for stiffness, strain and instability. Whether discomfort shows up on stairs, after sitting, during training or through longer walks and sport, this range is designed to support movement, reduce strain and help the joint feel more comfortable through daily activity.
See the knee support collectionBack
Lumbar supports and posture aids for lower-back discomfort, muscular fatigue and strain that builds through standing, lifting or long hours in one position. These products help add support, reduce effort through the lower back and make day-to-day movement feel steadier.
Discover back supportsShoulders
Shoulder supports for strain, overuse and movement that feels less controlled during reaching, lifting, carrying, overhead work or sport and training. This part of the range helps provide warmth, compression and a more supported feel while the shoulder settles and recovers.
Browse shoulder supportsWrists & Hands
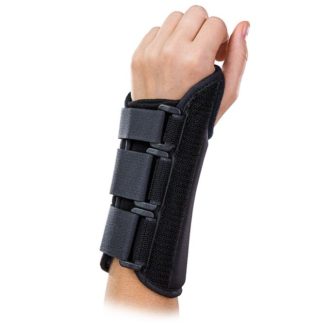
Wrist splints, hand supports and arthritis-friendly options for repetitive strain, gripping pain, hand fatigue and night-time tingling. These products are chosen to help limit irritation, improve support and make everyday tasks feel more manageable.
Explore wrist and hand supportsCompression & Leg Support
Compression sleeves, socks and lower-leg supports for tired legs, swelling, long periods on your feet, travel and active recovery. This range is designed to support circulation, reduce heaviness and help legs feel fresher through work, movement and recovery.
Find compression and leg supportSports Recovery
Recovery tools, resistance products and rehabilitation aids for training support, post-session recovery and a steadier return to activity. These products help you stay active with better preparation, better recovery and more support between sessions.
Shop sports recovery toolsBrowse by the Kind of Support You Need
Once you know which body area needs support and how symptoms tend to behave, the next step is choosing the right kind of help. Browse the full range below, organised by the type of support each product is designed to provide.
Footcare
Insoles, heel supports and footcare products chosen to reduce pressure, support the arch and make walking more comfortable. Whether the issue is heel pain, tired feet, underfoot strain or a need for better everyday support, this range is built to help you move more comfortably from the ground up.
Bodycare Supports
Braces, sleeves and structured supports that help steady joints and reduce strain during movement. From knees and ankles to backs, shoulders and wrists, this range is designed to add support where the body feels less secure, more irritated or under repeated stress.
Sports & Fitness
Recovery tools, training supports and rehabilitation aids for active people who want to protect movement, manage fatigue and recover well between sessions. Whether you are training regularly, returning from injury or building strength again, this range helps support performance and recovery in a practical way.
Why People Choose NuovaHealth
NuovaHealth is built around a straightforward idea: it is easier to choose the right support when you understand what your symptoms are actually telling you. That is why we focus on making product choice clearer, more practical and less overwhelming.
Instead of relying on vague promises, we organise support around what it is meant to do. That might mean reducing pressure through cushioning, improving stability around a vulnerable joint, adding compression to tired or irritated tissues, or helping protect an area that needs extra support during daily life, work or sport.
Most people don't arrive with a diagnosis. They arrive with a problem: heel pain in the morning, a knee that doesn't feel steady, an ankle that's never felt quite right since a sprain, or wrists that become painful after repetitive use. NuovaHealth is designed to help you start there and move towards a better-informed choice.
- A clearer way to browse We help you explore support by body area, symptom pattern and product purpose, so it is easier to narrow down what may genuinely suit your needs.
- A carefully chosen range Products are selected because they serve a clear practical purpose, whether that is cushioning, compression, bracing, stability or recovery support.
- Guidance in plain language We aim to explain products clearly, so you can understand what they are for, when they may help and how they fit into everyday life.
- Support for real-world movement Whether you are walking more, working on your feet, recovering from injury or staying active through training, NuovaHealth focuses on support that feels useful beyond the product page.
For some people, that means finding insoles that make everyday walking more comfortable. For others, it means a brace that adds confidence to a recovering joint, or compression that helps tired legs feel better through long days and active routines. Whatever brings you here, our aim is to help you choose with more confidence and less guesswork.
If you are not sure where to begin, get in touch. We are here to help you make sense of the options and find a more suitable place to start.
Understanding Pain Symptoms and How Support Can Help
Some people want a little more detail before deciding what to try. This section takes a closer look at common symptoms, when they tend to show up, why those differences matter, and how different kinds of support may help reduce strain, improve comfort or add stability.
Pain is not only about where you feel it. It also matters when it starts, how it feels, what seems to bring it on and which movements tend to make it worse. These details can give you a clearer picture of what part of the body is under strain. That is why something that helps one person may not be the best choice for someone else, even if the pain seems similar at first.
At NuovaHealth, we use these common signs and experiences to make product choice easier to understand. Cushioning may help by softening repeated impact and easing pressure on sensitive areas. Compression may help support tired or irritated tissues. Bracing may help steady a joint that feels vulnerable. More structured support can also help limit movements that tend to make symptoms worse while you stay active and recover.
That's why we start with body area, but don't stop there. Where pain shows up is only part of the picture. How it behaves, when it starts, and what makes it worse often matter just as much when choosing the right kind of support.
Sharp pain on your first steps that eases as you walk often happens when tissue under the foot tightens while you rest, then stretches suddenly when you stand up. This is a common pattern with irritation of the plantar fascia, the band of tissue that runs along the sole of the foot. Support may help by reducing that stretch, supporting the arch of the foot and softening pressure through the heel so walking feels less aggravating.
Pain that gradually builds while you are active and is still there afterwards often points to a body part being asked to do more than it is coping with comfortably. That might involve a tendon, a joint that is not moving smoothly, or muscles that are working harder than they should. In this situation, support may help by spreading pressure more evenly, reducing excess movement and making activity easier to manage.
A joint that feels unsteady or as if it might give way often means you are dealing with both reduced control and reduced confidence in that area. This is common after a sprain, especially if stretched ligaments are no longer giving the joint the same sense of position and movement as before. A support may help by adding external stability and by improving awareness of the joint through gentle compression and contact around it.
Stiffness that is worse after rest and eases once you get moving is often noticed when a joint is irritated, not moving enough, or affected by age-related wear. Movement can help the joint feel looser again, while support may add warmth, light compression and a greater sense of security during activity.
Tingling, numbness or a burning feeling can suggest that a nerve is being irritated or squeezed somewhere along its path. For example, a wrist splint may help keep the hand and wrist in a better position during sleep, while a back support may help some people feel more comfortable by reducing strain around the lower back.
Small differences in symptom pattern often matter more than people expect. Pain under the heel that is worst on first steps is not always asking for the same kind of support as soreness that builds after a long day on hard floors. A knee that feels stiff after sitting may need something different from one that feels less stable on stairs or uneven ground. An ankle recovering from a recent twist may need a different level of support from one that has felt unreliable for months.
That is why support works best when it is matched to the job it is trying to do. In some cases, the aim is to cushion repeated impact. In others, it is to reduce excess movement, improve confidence in a joint, spread pressure more evenly or make everyday activity easier to manage while irritated tissue settles. Looking only at the body part is often not enough. How the problem behaves usually adds the detail that makes a better choice possible.
Support usually works best alongside sensible choices about activity. That does not always mean stopping completely. Often, too much rest can leave muscles weaker and joints stiffer. A better approach is usually to cut back on what clearly makes symptoms worse, keep moving within comfortable limits and use support to make everyday activity feel more manageable while things settle.
For example, if pain under your heel is worst when you first get out of bed, supportive insoles may make walking easier while you also work on stretching tight calf muscles and avoid sudden increases in walking or exercise. If your ankle still feels unsteady after a sprain, a brace may help you move with more confidence while you rebuild balance and strength. If wrist discomfort builds through gripping, lifting or repeated hand use, a splint or support may help reduce aggravation while the area settles.
Support is there to help you through a problem, not to do everything on its own. In many cases, it works best as part of a broader approach that may also include exercises, a gradual return to activity and better day-to-day management of how much strain the area is under.
If symptoms are not improving, keep coming back, or feel more severe than a simple strain, getting the right assessment matters. Support can be useful, but it is not a replacement for proper advice when something needs closer attention.
Common Pain Patterns and How Support May Help
Use the guide below to explore common patterns by body area, understand what may be contributing to the problem, and see how different forms of support are typically used. It is a practical reference designed to help you browse the range with a clearer sense of what might suit you.
A quick note before you browse: these summaries are here to help you recognise common patterns and understand why certain types of support are often recommended. They are intended as general guidance rather than diagnosis.
If your symptoms are severe, sudden, unusual or not improving, it is always best to seek proper assessment from a qualified healthcare professional.
What you might notice
Heel pain often feels sharpest on the first steps of the morning or after rest. Once you have moved around for a few minutes, it may ease into a dull ache, only to return again after longer periods on your feet, walking or running. This is one of the most common patterns seen with plantar fascia irritation.
The plantar fascia is the thick band of tissue running along the underside of the foot from heel to toes. It helps support the arch and manage the load created every time you walk, stand or push off.
Why your foot hurts
When the plantar fascia is repeatedly overloaded, it becomes irritated. During rest, especially overnight, the tissue can tighten slightly. That is why the first few steps often feel the worst. As the foot warms up, the pain may ease, but the underlying strain is still there and often returns later in the day.
Common contributors include poor arch support, tight calves, sudden increases in walking or running, long periods on hard surfaces and footwear that does not absorb pressure well.
What often makes it worse
This type of heel pain is often aggravated by long shifts on hard floors, barefoot walking on unforgiving surfaces, unsupportive shoes and sudden increases in activity. For some people, it is worst after rest. For others, it starts that way but also builds again after a busy day, especially when the foot has had to absorb repeated impact without enough support.
It is also common for people to notice that discomfort under the heel is not the whole story. The arch may feel tight, the sole of the foot may ache after longer periods standing, and calves may feel stiff if they are contributing to the overall pull through the heel.
How the right support can help
Insoles and heel cups help reduce the pull on the plantar fascia and soften impact under the heel. Arch support lifts the middle of the foot, which can reduce strain through the fascia with each step. Cushioning helps spread pressure more evenly instead of concentrating it in the heel.
A heel cup may suit people mainly looking for softer landing and more comfort directly under the heel, while a full-length insole may suit those who also need better arch support and more balanced pressure through the whole foot. Which feels more useful often depends on whether the main issue is heel impact, arch strain or a mixture of both.
What support cannot do on its own
Support can make walking feel more manageable, but it usually works best when the overall strain on the foot is also addressed. If walking volume keeps rising, footwear remains unsupportive or calf tightness is never worked on, symptoms often continue to return even if support helps in the short term.
Why this matters
If heel pain is ignored, people often start limping or changing the way they walk to avoid discomfort. That can affect the ankle, knee, hip or lower back over time. Appropriate support, used alongside stretching and sensible activity changes, can help break that cycle.
When to seek professional help
Seek further assessment if heel pain is severe, getting worse, not settling with support and activity changes, or comes with numbness, marked swelling or symptoms that do not fit a typical strain pattern.
What you might notice
Achilles pain often feels stiff and sore first thing in the morning or after sitting still. Once you have walked for a few minutes, it may loosen up, but then return during or after activity, especially running, jumping or walking uphill. The tendon may also feel tender, thickened or slightly swollen.
Some people notice that the tendon feels manageable once they warm up, only to become more irritable later in the day or the following morning. That pattern of easing, then returning, is common when the tendon is being asked to cope with more load than it currently tolerates comfortably.
What is happening in the tendon
The Achilles tendon connects the calf muscles to the heel and handles very high loads during walking and sport. When the tendon is repeatedly stressed beyond what it can currently tolerate, it becomes irritated. This may happen after a sudden jump in training, repeated overload or a long period of pushing through discomfort.
Stiffness in the morning is especially common because the tendon can feel more reactive after rest, then loosen slightly as it starts moving and warming up again. That does not always mean it is recovering well. In many cases, it simply means the tendon is settling temporarily before being stressed again.
What tends to aggravate it
Achilles pain is often made worse by uphill walking, sprinting, jumping, quick increases in running volume or returning to sport too fast after time off. Shoes with very flat or unsupportive soles may also leave the tendon working harder than it is ready for, especially during a more reactive phase.
Even outside sport, people often notice it during stairs, longer walks or when they have been on their feet for hours without much recovery between days.
How support and heel lifts can help
Compression supports can help the tendon feel more secure and may reduce swelling around the area. Heel lifts slightly reduce how far the Achilles has to stretch with each step, which can be helpful when symptoms are especially reactive.
Used sensibly, this kind of support can make day-to-day movement more comfortable while the tendon settles. It is usually best thought of as a short-term aid alongside appropriate loading and calf strengthening.
A softer compression sleeve may suit people mainly looking for a more supported feel and mild symptom control through daily movement, while a heel lift may be more useful when the main problem is stretch sensitivity through the tendon during walking.
What support cannot do on its own
Support may reduce irritation and make movement easier, but it does not rebuild the tendon's load tolerance by itself. If the tendon is repeatedly flaring because training, walking volume or intensity keeps rising too quickly, symptoms often return unless the loading pattern is also addressed.
Why this matters
Achilles problems can become stubborn when they are repeatedly aggravated without enough recovery or support. Early management often makes it easier to keep moving without letting the problem drag on.
When to seek professional help
Get urgent assessment if you feel a sudden sharp pain with a popping sensation or immediate weakness through the tendon. Persistent Achilles pain that is not improving usually benefits from proper rehabilitation guidance.
What you might notice
Calf pain can feel tight, cramping or suddenly sharp if the muscle has been strained. Shin splints usually feel like an aching discomfort along the shin, often worse during or after running, walking or impact exercise. Some people also notice heavy, tired legs after long periods standing, travelling or training.
For some, the discomfort is mainly about muscular fatigue and heaviness. For others, it is more localised and repetitive, especially if impact activity has increased quickly or the lower leg has been asked to absorb more force than it is used to. The exact pattern matters, because general tiredness behaves differently from a more reactive strain pattern.
What may be under strain
The calf muscles handle a large amount of force during walking and especially during running and jumping. Shin pain often develops when the muscles and tissues around the shin are repeatedly overloaded, particularly after a rapid increase in activity or when foot mechanics place extra stress through the lower leg.
In some cases, the issue is not a single injury but a gradual build-up of load. Tissues that cope reasonably well at one training level can become irritated when distance, pace, hill work or standing time increase faster than recovery allows.
What tends to aggravate it
Lower-leg symptoms are often aggravated by running on hard ground, steep hills, long days on your feet, sudden jumps in training volume, poor recovery and footwear that no longer offers enough support or shock absorption. Standing still for prolonged periods can also leave the calves feeling heavy and more sluggish by the end of the day.
Where shin splint-type symptoms are involved, repeated impact without enough progression is one of the most common patterns. In more muscular cases, fatigue often becomes more obvious later in the day, after sport or after prolonged standing.
How compression can help
Compression sleeves can support the calf and lower leg, help manage swelling and reduce the feeling of heaviness through tired muscles. For some people, they also make movement feel more controlled during exercise or recovery.
A lighter compression sleeve may suit people mainly looking for support during longer days on their feet, travel or active recovery, while firmer compression may feel more useful during training or when the leg feels especially heavy, reactive or unsupported.
What support cannot do on its own
Compression can improve comfort and help the lower leg feel fresher, but it does not remove the need to manage training load, footwear or recovery. If the same aggravating pattern continues without adjustment, lower-leg symptoms often keep returning even when support helps temporarily.
Why this matters
Repeated calf or shin pain can become difficult to manage if the underlying load is never adjusted. Appropriate support, better progression of activity and attention to footwear or movement habits can all help prevent symptoms from building into a more persistent problem.
When to seek professional help
Seek urgent advice if calf pain comes with unusual swelling, redness or warmth, or if shin pain becomes very localised and severe. Symptoms that do not settle with reduced load should also be properly assessed.
What you might notice
After a sprain, the ankle may start with sharp pain, swelling and difficulty putting weight through the foot. Even once the worst of that settles, it is common for the joint to feel unreliable, especially on uneven ground, during quick changes of direction or when returning to exercise.
Some ankles no longer feel actively painful most of the time, but still feel unstable, hesitant or vulnerable in the moments that matter. People often describe this as the ankle not feeling fully trustworthy, even months after the original injury.
What has been affected
Ankle sprains usually involve stretching or tearing the ligaments that stabilise the joint. The body can also lose some of the normal feedback that helps it sense joint position, which is why the ankle may still feel wobbly even after the initial pain improves.
That reduced confidence is not only psychological. A previously sprained ankle often becomes less accurate at sensing movement and position, which can make the joint feel slower to react when you step awkwardly or change direction quickly.
What tends to aggravate it
Instability is often most noticeable on uneven pavements, trails, slopes, stairs, busy days on your feet or when returning to sport before strength and balance have fully recovered. Some people also notice it when they are tired, because the muscles helping stabilise the joint are no longer reacting as well as they do earlier in the day.
This is one reason repeat sprains are so common. The ankle may feel almost normal in simple walking, but much less dependable when speed, fatigue or awkward footing are added.
How ankle support helps
Ankle braces and supports can limit excessive rolling, improve the feeling of stability and help protect healing structures while you regain confidence. Compression around the joint may also improve awareness of ankle position, which can help balance and control.
Different levels of support suit different stages. Some people need firmer support early on, then something lighter as strength and confidence return. A softer sleeve may suit mild weakness and day-to-day reassurance, while a more structured brace may suit sport, uneven ground or a recent return to activity.
What support cannot do on its own
A brace can help protect the ankle and make movement feel safer, but it does not fully replace the need to rebuild balance, control and strength. If the ankle is repeatedly protected without ever retraining its ability to stabilise well, the same instability often returns when support is removed.
Why this matters
Ankles that are not properly supported and rehabilitated after a sprain are more likely to be sprained again. Repeated instability can become a long-term issue if the joint never fully regains control.
When to seek professional help
If you cannot bear weight, if pain is severe, or if swelling and bruising are significant, proper assessment is important. Persistent instability after a sprain should also be looked at more closely, especially if the ankle keeps rolling or never feels fully reliable again.
What you might notice
Knee pain can show up in different ways depending on what is being irritated. Pain around the kneecap often gets worse with stairs, squatting or sitting for too long. Some knees feel stiff after rest, while others feel weak, wobbly or less controlled during walking and exercise.
People often describe the knee in different terms depending on the pattern. Some talk about an ache at the front of the knee, especially with bending. Others notice swelling, tightness, clicking, a feeling of poor control or a sense that the joint is not moving as smoothly or reliably as it should.
What may be under stress
The knee relies on a combination of ligaments, muscles and joint surfaces working together smoothly. Pain may come from poor kneecap tracking, overload through the surrounding muscles and tendons, swelling inside the joint or a sense of instability after injury.
Not all knee pain points to the same kind of problem. A knee that is painful mainly on stairs or after sitting can behave very differently from one that feels unstable during turning, uneven ground or longer walks. That is why the way symptoms show up often matters just as much as the place you feel them.
What tends to aggravate it
Knee symptoms are often aggravated by stairs, squatting, kneeling, longer walks, repeated standing up and down, and exercise that increases load faster than the joint is ready for. Sitting still for long periods can also make some knees feel stiff and uncomfortable, especially if the kneecap area is already irritated.
Where instability is part of the picture, quick direction changes, slopes and uneven surfaces often make the problem more obvious. Tired muscles around the hip and thigh can also leave the knee feeling less supported later in the day.
How knee supports can help
Compression sleeves can help reduce swelling, improve comfort and give the knee a more supported feel during movement. More structured braces can offer extra stability where the joint feels less reliable. Some designs also help support the kneecap or reduce strain through the tendon below it.
A lighter sleeve may suit people looking for warmth, mild compression and a more confident feel during day-to-day activity, while a firmer brace may be more useful where there is clearer instability, post-injury weakness or a need for more support during activity.
What support cannot do on its own
Support may help the knee feel steadier and more comfortable, but it does not remove the need to improve strength, movement control and loading where those are part of the problem. If the knee is repeatedly being pushed into aggravating movement without enough recovery or rebuilding around it, symptoms often return.
Why this matters
When knee pain is left to build, people often move differently to protect it, which can put extra stress elsewhere. Appropriate support can help make movement feel safer and more comfortable while strength and control are rebuilt.
When to seek professional help
Further assessment is important if the knee locks, gives way repeatedly, becomes significantly swollen, or stays very painful despite rest and support.
What you might notice
Lower back pain often feels like stiffness, tightness or a dull ache that builds through standing, sitting, lifting or bending. Some people feel it most after long periods in one position, while others notice it more after repeated movement or heavier tasks.
For some, the back feels tired and vulnerable by the end of the day. For others, it flares more suddenly after awkward lifting, repeated bending or spending too long in one posture. It may feel local and muscular, or it may spread into the buttock or upper leg as the area becomes more irritated.
What may be under strain
The lower back supports the weight of the upper body while allowing a wide range of movement. Muscles, ligaments, joints and discs all share that load. When one part is irritated or the area becomes fatigued, the back may feel tight, vulnerable or more easily aggravated.
That does not always mean something serious has happened. In many cases, the back has become overloaded, fatigued or more sensitive than usual. Even so, the effect on confidence and day-to-day movement can be significant, especially if the area starts feeling unreliable whenever you bend, lift or stay in one position too long.
What tends to aggravate it
Back pain is often aggravated by long periods sitting, repeated bending, lifting, twisting, standing for too long without support, or returning too quickly to demanding physical tasks. Some people notice that the problem is less about one big movement and more about cumulative fatigue building through the day.
Others find that flare-ups happen when they have done too little movement for too long, then suddenly ask the back to do more than it has recently been used to. That pattern of stiffness followed by reactivity is very common.
How back supports can help
Lumbar supports can add compression, warmth and a greater sense of support through the lower back. They may help reduce strain during flare-ups, long periods on your feet or activities that would otherwise make symptoms worse.
For some people, the biggest benefit is not dramatic pain relief but improved confidence. The support can make movement feel more controlled, reduce the sense of vulnerability around the lower back and make it easier to get through work, travel or busy days with less irritation building up.
What support cannot do on its own
Back supports are usually most helpful as part of a wider approach, not as the only answer. They can make day-to-day activity easier, but they do not replace the need to improve movement tolerance, rebuild strength where needed and manage the amount of strain being placed through the area.
Why this matters
Back pain can become persistent when the area is repeatedly irritated without enough support or sensible pacing. Temporary support can help you stay active without constantly aggravating the problem, which is often more useful than swinging between overdoing things and resting completely.
When to seek professional help
Urgent assessment is needed if back pain comes with major weakness, changes in bladder or bowel control, or unusual numbness. Ongoing pain that is severe, worsening or spreading further down the leg also needs proper attention.
What you might notice
Wrist and hand problems often show up as aching, tingling, numbness or weakness during and after repetitive tasks. Night-time tingling, especially through the thumb and first fingers, is a common pattern in carpal tunnel problems. Others notice pain after gripping, lifting or repeated hand use.
Some people mainly notice symptoms after long periods of activity, while others are bothered most at night or first thing in the morning. In some cases the wrist feels weak, clumsy or tired rather than sharply painful, especially if irritation has been building over time.
What may be irritated or compressed
Some symptoms come from irritated tendons and overworked forearm muscles. Others involve compression around a nerve, particularly through the carpal tunnel at the wrist. Repeated hand and wrist positions can gradually build irritation over time.
This is why two people with wrist pain may need different kinds of support. One may mainly need the joint held in a calmer position at night. Another may need light daytime support to reduce irritation during repetitive tasks. Another may simply need help limiting aggravating positions while symptoms settle.
What tends to aggravate it
Wrist symptoms are often aggravated by long periods gripping tools, lifting and repetitive hand use. Night-time symptoms often become more obvious because the hand and wrist stay in one position for long periods without you realising.
People also commonly notice that discomfort builds gradually rather than suddenly. The more often the same hand and wrist positions are repeated without enough variation or recovery, the more likely irritation becomes.
How wrist supports can help
Wrist splints can hold the joint in a more neutral position, which may reduce pressure around irritated structures and make night-time symptoms easier to manage. Compression and light support can also help calm irritation during repetitive tasks or recovery.
A firmer splint may suit night-time symptoms, tingling or a stronger need to limit movement, while a lighter support may suit daytime use where the aim is to reduce aggravation without fully restricting the hand.
What support cannot do on its own
Support may reduce irritation and improve comfort, but it will not fully solve a problem if the hand is still being pushed through the same provoking tasks without any change in load, position or recovery. Symptoms often improve faster when support is combined with more sensible pacing and less repeated aggravation.
Why this matters
Symptoms that are ignored can become harder to reverse, especially if they start affecting grip, sleep or everyday hand use. Early support and sensible changes in load can make a meaningful difference.
When to seek professional help
Persistent numbness, worsening weakness or symptoms that are affecting hand function should be assessed properly, especially if they are no longer settling with rest or support.
What you might notice
Shoulder pain often feels like a deep ache that gets worse with reaching, lifting or overhead movement. Some people notice discomfort when putting on clothing, carrying bags or sleeping on the affected side. Others feel weakness, catching or a loss of smooth control through certain movements.
For some, the shoulder mainly feels painful in certain positions. For others, it feels less reliable, less controlled or more tiring during repeated use. It is also common for the area around the upper arm, front of the shoulder or shoulder blade to feel tense as the body starts guarding the movement.
What may be under stress
The shoulder depends on good coordination between muscles, tendons and joint position. When those tissues are overloaded, irritated or less well controlled, movement can become uncomfortable and less stable. Rotator cuff irritation is one of the most common examples.
Because the shoulder is designed for mobility, it can also become sensitive when it no longer feels well centred or well controlled during movement. That is one reason symptoms often show up during reaching, lifting away from the body or repeated overhead use rather than during simple rest alone.
What tends to aggravate it
Shoulder symptoms are often aggravated by lifting, reaching above shoulder height, carrying, repeated pulling, gym work, awkward sleeping positions and tasks that keep the arm away from the body for long periods. Repetitive work and sport can also make symptoms gradually worse, especially when the shoulder has not fully recovered between sessions.
People frequently notice that once the shoulder becomes irritated, everyday tasks start to matter more than expected. Putting on a coat, reaching into cupboards, washing your hair or carrying shopping can all begin to trigger discomfort if the area is already reactive.
How shoulder supports can help
Shoulder supports can provide warmth, light compression and a more supported feel during daily activity. Some designs also help improve posture or reduce the sense of strain around the joint. In some cases, limiting aggravating movement slightly can help the shoulder settle while you stay active within reason.
A lighter support may suit people looking for warmth, reassurance and symptom control through daily tasks, while a more structured design may feel more useful where the main problem is poor control, repeated strain or a need for better movement awareness.
What support cannot do on its own
Support can make movement feel more manageable, but it cannot fully restore strength, control or shoulder tolerance on its own. If the shoulder is repeatedly pushed into provoking movement without enough adjustment in load or activity, symptoms often keep returning.
Why this matters
Shoulder problems often become more frustrating the longer they are repeatedly irritated. Pain can lead to guarding, reduced movement and further weakness, making everyday tasks harder than they need to be.
When to seek professional help
Get proper assessment if shoulder pain starts suddenly after injury, if weakness is significant, or if symptoms are not improving with sensible changes and support.
Ready to Find the Right Support?
Whether you're managing everyday discomfort, recovering from injury or looking for better support during training and sport, NuovaHealth helps you choose with more confidence and less guesswork.
Evidence-Based
Selection
Selection
Carefully Chosen
Range
Range
Helpful Support
Available
Available
Fast UK
Delivery
Delivery